Initiating and Maintaining Support Groups in Liver Clinics - Hepatitis C
Objectives and Structure
With newer treatments available, hepatitis C is now curable and treatment is much easier to complete. The type of support group used to help patients engage in treatment in the past may no longer be needed for most patients. However, different types of group programming may be useful in maintaining liver health, managing cirrhosis, or addressing healthy lifestyle changes.
What does a group provide?
- Group cohesion. Feelings of trust and safety are primary benefits of group affiliation, as is the recognition of the universality of one's problems, which decreases feelings of personal isolation.
- Education. Interpersonal learning is exchanged in group settings, and increased knowledge about liver health and liver disease is the first step toward successful self-care and evaluation of treatment options.
- Discussion. Veterans learn as much from each other as they do from providers and staff. Creating an opportunity for dialogue facilitates this exchange of information.
- A venue for expression of needs. Providers can learn what Veterans feel they need to help them manage and cope with liver disease.
- Prevention. Alerting Veterans and caregivers to behavioral risk factors can help limit transmission or reinfection of hepatitis C or disease progression for other liver diseases.
- Opportunity for follow up. Weekly or even monthly participation in a group allows providers to continue monitoring patients informally and reinforce important messages for effective self-care.
Steps in Group Development
Here is a general outline of the steps involved in developing a group. Each of these steps is expanded below:
- Conduct a needs assessment
- Identify target population
- Select group format
- Identify resources
- Attend to logistics
- Establish your group
- Implement a feedback function
1. Conduct a Needs Assessment
A formal or informal needs assessment is essential to help with decisions you will have to make about group focus, format, meeting time, location, and group size. This needs assessment may range from a written survey of your patients to simply engaging several individuals in a discussion about what they would find helpful. As a start, you might use a variation of the support group feedback form contained in Appendix E to find out about patients' interests.
Asking patients what they need is important; do not assume that you already know what they want. Collect information about both the content of the group meetings (e.g., topic interests) and logistics (e.g., where, when and how often to meet). Veterans will have differing opinions as well, so you will have to go with what appears to meet the greatest need for the greatest number of patients. You can also talk with Hepatology providers about their impressions of their patients' presenting concerns and how a group could help them.
NOTE: It is important to give yourself enough time to set up your new group. Try to allow for a 3-month lead time. It takes time to contact patients, and you will want to allow an adequate time frame to get the word out and attend to the details of establishing a new group.
2. Identify Target Population
Who are the intended participants of the group? This is the first and probably the most important decision to make. On the basis of your needs assessment, you will have to decide who would benefit most from group participation. For example, your group may target:
- Patients who have not yet engaged in hepatitis C treatment
- Patients awaiting transplant or post-transplant disease management
- Patients with HCC (hepatocellular carcinoma) or other serious liver related illness
- Patients with cirrhosis working on disease management
- Patients with NAFLD working to lose weight
- Veterans only, or Veterans and family members
How many patients do you plan to invite? Your target population and selected group format largely will determine this. You may decide to start with a very specific target population for your first group, then use that experience to either expand your group or start other groups.
3. Select Group Format
There are a variety of group formats to consider. The most relevant dimensions for groups are structure, size, and focus (i.e., process-oriented vs. didactic in focus). A process-oriented group is one in which attention is focused more on individual members' concerns, thoughts, and feelings rather than on topical information provided by an "expert." The three dimensions mentioned are illustrated in the following figure:
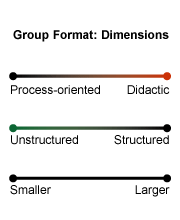
The group format you select will depend largely on patient needs and your available resources. Below are several general categories of groups. Your group may be a hybrid or modification of these types.
Support Group
- Objective: At a minimum, these groups provide opportunity for social interaction.
- May be loosely defined, although participants usually share some characteristics.
- Benefits: Vicarious learning, sharing of resources.
- Can be:
- Patient-led, peer-led or provider-led
- Process-oriented or topic-oriented
- Predefined or ad hoc topic, based on the needs of the members
- Process groups are less structured, but no less challenging to ensure effectiveness (see information under "Therapy Group" below).
- Size of group: 8-12 members optimal for process-oriented group.
- May be open to family members.
- Example: Group for patients trying to lose weight
Education-oriented Group
- Objective: Learning more than mutual support.
- Organized around a topical objective.
- Often a series of meetings of defined duration.
- Topics established in advance.
- Topical expert leads the presentation, although a facilitator usually is also present.
- Social support is a byproduct rather than a primary goal.
- Usually open to family members.
- Example: Guest lectures for patients with cirrhosis and their family members
Therapy Group
- Objective: Mental health intervention.
- Led and facilitated by a mental health professional.
- Size limited depending on nature of group.
- May be either ongoing or time-limited.
- Usually organized around common diagnosis or diagnoses among patients.
- Usually closed to family members or others.
- Example: Psychotherapy group for patients with both post-traumatic stress disorder and liver disease
Recovery Group
- Objective: To promote and maintain abstinence from substance use.
- Focused topic and/or mutual support (e.g., Alcoholics Anonymous, CODA [Co-Dependents Anonymous]).
- Usually ongoing.
- Drop-in approach common.
- Example: Group for patients with hepatitis C recovering from opioid/substance abuse, intravenous drug use
Hybrid/Combination Group
-
May involve a dual population
- HIV/HCV co-infection (note: may require specific informed consent prior to group start)
- HCV and addictions treatment
-
May be a dual-purpose group or involve splitting the session to address multiple goals
- Education plus support
- Support plus therapy
4. Identify Resources
It may be helpful to have two facilitators for a group, with one being a VA staff person or a professional and the other, if possible, a peer facilitator.
Co-facilitation
Using two facilitators in any group has several advantages:
- While one facilitator is taking a more active role by speaking to or facilitating the group, the other facilitator can attend to the process or system issues of the group, making note of follow-up issues for after the group meeting and offering a crucial second point-of-view.
- Having two facilitators offers a chance to model positive interpersonal skills: facilitators can openly disagree on subjects and demonstrate constructive resolution.
- Practically, having two facilitators means the group can continue even on days when one facilitator is absent.
Choosing a Second Facilitator
We strongly encourage having at least one peer facilitator for the group. Many Veterans may prefer leadership from another Veteran who also has experience with the disease (cured of HCV, currently has cirrhosis for example). Some Veterans see a peer as a more credible source of information than a professional. Ideal peer facilitators are often patients who have already assumed some type of advocacy role regarding their health care or the care of other Veterans. You may want to consider differences in Veteran experience as well when selecting a peer. For example, if the group will mostly be younger Veterans it can be beneficial to have a Veteran in that age group as facilitator. Peer facilitators can be recruited by providers, at educational events, through local Veterans service organizations, etc.
Having a professional facilitator ensures that the interpersonal aspects of the group are therapeutic, regardless of the group's type. The professional facilitator should train and mentor the peer facilitator in developing basic group skills just as the peer facilitator should train and mentor the professional facilitator in the personal experience of liver disease. This training can be formal or informal, but the most important learning occurs with continuous feedback and discussion with debriefing after group sessions. We recommend training peer facilitators in at least the following areas:
- Communication skills: e.g., "I" statements, empathy, active listening
- Motivational interviewing: e.g., developing discrepancy, rolling with resistance
- Basic group and system principles and interventions: e.g., group roles, group developmental stages, fostering cohesion
- Facilitation strategies and techniques: e.g., redirecting, rewarding group behavior, handling disruptive behavior, tolerating awkward silences
Please consult Appendix D for elaboration on these topics.
Flexibility
All that being said, groups can be successfully run by one or two facilitators, peer or professional. In areas with limited VA resources, a group organizer may have to find creative ways to start a group using community resources. Although VA professional facilitators may be unavailable to lead a group, they still may have the time to mentor peer facilitators, individually or as a team, in group skills. Having a well-run therapeutic group that addresses patients' needs is more important than adhering to a predetermined format for which there are no local resources.
Security
Peer facilitators should be approved VA volunteers who have gone through appropriate orientations and safety checks to ensure patients' safety, confidentiality, and well-being.
Roles
It is crucial that before the group begins, the facilitators agree on their roles and how they will manage the group together. Facilitators may decide to be completely equal in leadership and division of labor or to divide their responsibilities differently: one facilitator may be the leader while the other plays a more secondary role, or one may be in charge of the group's process while the other is in charge of the content. How the responsibilities are divided is not as important as having the division clear and agreed on by the facilitators. When a volunteer or peer facilitates, the professional facilitator or other VA employee should make clear to members the boundaries on the volunteer's participation.
Guest Speakers
Early on, start building a list of contacts to use as potential speakers at your meetings. Keep in mind that many speakers need several months' lead time to commit to a specific date or time. Some guest speakers may require compensation.
Speakers should possess a thorough knowledge of the topic or their specific content area. Speakers whose presentations you have attended and enjoyed and those who are adept at drawing people into discussions are best to invite. You may also want to consider having physicians, nurses, social workers, or psychologists attend the group sessions from time to time (or as guest speakers) to act as further resources for the group. Ideally, these individuals should have experience in the area of liver disease or in treating serious illness. Many patients have indicated particular interest in certain topics. Support group planners may seek out guest speakers with specialized knowledge or expertise in these areas. (See Appendix F for suggested topics.)
The American Liver Foundation
The American Liver Foundation (ALF) is a resource for starting groups, particularly if your group is to be based in the community rather than at a VA medical facility. ALF has an expert speakers' bureau and provides many helpful suggestions for structuring and conducting your support group. You may wish to contact ALF and work together once you have an idea as to the purpose and target population of your group.
Industry Support
Corporations that develop health care products and services sometimes offer resources that can benefit your group, such as informational materials on hepatitis C and patient care consultants who can serve as speakers. VA rules prohibit soliciting support from industry representatives, but donated support, such as unrestricted educational grants, may often be used to augment the resources available from your facility. Many VA medical centers have specific policies or procedures pertaining to acceptance of support from outside sources, and you should make sure that you understand and abide by these. Representatives of outside organizations that provide support should not be permitted to attend patient support groups.
Community Resources
One mission of this manual is to help group facilitators empower Veterans with knowledge and resources that promote optimal self-care. To increase information access, we suggest you provide Veterans with a resource list addressing their varied concerns. This list could include the following:
- Contact information on agencies and websites that promote liver health, education, and advocacy
- Relevant case management and social service resources (e.g., legal aid, Social Security, housing, Americans with Disabilities Act, and disability rights contacts)
- Recommended readings on liver health, hepatitis C, and related issues (Many resources available on www.hepatitis.va.gov)
- Information on current liver research
- Public health clinics and other locations that test for hepatitis (especially for significant others)
- Advocacy organizations
- Other support groups in the community
- Contact information on alcohol and drug recovery resources
5. Attend to Logistics
Planning
- When are most participants available?
- When is the facility available?
- How frequently will people be able to meet (weekly, monthly)?
- Is there adequate parking?
- Is there access to audiovisual equipment?
- Is the room arrangement and number of chairs sufficient for the group?
- Who will be responsible for opening and closing the facility?
Location
Once you have an idea of when and how often your group will meet (at least for the first couple of meetings) you need to secure a location for the group. Ideally, you will have meeting space at your VA facility. The space should be large enough to seat everyone comfortably, but if the space is too large it may feel cold and impersonal for the purpose of the support group.
If you have to hold your support group offsite:
- Some locations may require payment for use of the facility.
- Contact community resources (e.g., library, town hall) or community organizations (American Red Cross, Rotary Club, Lions Club, YMCA/YWCA, Salvation Army).
- Most organizations have community relations offices as a contact point.
- Also consider local hospitals, health centers, a doctor's office, or the local Visiting Nurses Association.
- Have an idea of the total number of meetings and/or the number of months you plan to meet prior to making the initial contact call (most meetings last approximately 11/2 hours, plus time for questions).
- Don't forget time for setup (refreshments, video, etc.) and cleanup.
- Let your point of contact know projected dates and times, that the meetings are free of charge, and that the group is voluntary and nonprofit.
Wherever you hold your group, be sure to consider safety issues (adequate lighting, in a safe area), especially for night groups, to minimize the possibility of harm to or harassment of participants. Also consider confidentiality issues when creating your signs for the support group. For example, Liver Support Group would likely be preferable to Hepatitis C Support Group when posting signage.
Establishing a Clinic in CPRS for the Group
One important step in developing your group is to set up one or more clinics in the Computerized Patient Record System (CPRS), in order to capture accurately the workload data associated with the group. This should be done before the groups begin but near the end of the planning process.
To set up a clinic in CPRS you will need the following information:
- The length of each group session
- The primary provider(s) associated with the group sessions
- Other providers who will be routinely speaking to the group
You will need to work with your station's Decision Support Service (DSS) program manager or analyst, or other staff responsible for creating clinics in CPRS. Find appropriate staff to help you identify and set up the primary and secondary stop codes within that clinic as well as local codes to capture every element of the workload associated with the group. You may need only one clinic to capture the workload or you may need several, depending on the providers associated with the group. Please advise the person assisting with the clinic setup that Veterans attending these clinics must not be charged for the visit.
There may be other considerations for setting up a clinic at your facility. Some facilities may require a review of patient education materials. Others may have a system for reimbursement of travel costs for attending the meeting. Any requirements for individual facilities should be addressed ahead of time, and the process should be in place prior to the first meeting.
Referral Process
How you select and bring people into the support group will vary depending on its format and objectives. Each method has advantages and disadvantages, as indicated below.
View table
Providers can be the best referral source for potential group participants. They often know the patients' needs as well as their current health status. Discuss who might benefit from group participation with physicians (especially gastroenterologists, hepatologists, and infectious disease specialists), nurses (especially those who treat liver disease), social workers, psychologists, and other mental health professionals (especially those who work with patients with a history of substance abuse and/or chronic disease).
If you send invitations to patients by mail, our early experience with this method resulted in a 10 to 20 percent attendance rate among those we invited. If you call selected patients by phone, your response rate likely will be higher, and you will also have a greater sense of who will attend by what they tell you.
Meeting Logistics
A meeting planning tool is enclosed (see Appendix B) to help keep track of what has been done and what needs to be done for each meeting, once your meetings are under way. Here are some considerations for your first group and beyond:
- Audiovisual. Do you have the equipment that you or your guest speaker needs for a presentation (e.g., VCR, PowerPoint, overhead projector)?
- Food/Refreshments. Food helps to attract and maintain group participation. If possible, provide food that is healthy for patients with liver disease (i.e., avoid high-sugar sodas and caffeinated beverages). If you serve food, remember the little things everyone needs (napkins, utensils, serving spoons).
- Directions/Signs. Patients will easily get frustrated if they have to walk the length of the hospital to find the meeting room.
- Announcements. Groups are great forums for disseminating information, especially information about upcoming meetings and speakers.
- Handouts. Do you have enough copies? Are large print versions needed?
- Brochures/Flyers. See "Community Resources" section above.
- Room Environment. Check temperature, lighting, and seat arrangement in advance. You may need to obtain a key beforehand to gain access to the room.
- Name Tags. Do you want people to wear them or not?
6. Establish Your Group
Guidelines
Having some general guidelines and expectations regarding group conduct established from the beginning can make the group more comfortable for the members. This will help to resolve difficult situations without appearing dictatorial. Appendix C is a list of patient rights and responsibilities you may wish to incorporate. In your first meeting, ask group members for help in generating this list to create buy-in.
Confidentiality
At the first meeting it is a good idea to establish and emphasize that every member should respect the confidentiality and anonymity of individual group members. Your group may also decide if it is to be open or closed to spouses, family members, or friends. Group members should feel free to express themselves without fear that their private lives will become a matter of public knowledge outside the group.
Mission Statement
To begin, prepare a mission statement for the first meeting (see sample in Appendix A). Ask members to suggest changes or additions. With their input and feedback, you will be able to ensure that the interests and needs of the group will be met. You should review this mission statement periodically to help the group stay focused on its purpose and goals.
Potential Problem Areas
Facilitating a group, large or small, can be tricky. The following table lists common problem areas that often arise in groups, along with some suggested remedies. We suggest you read Appendix D to learn more about group facilitation. Many of these tools may come in handy once the group starts.
| Problem | Solution |
|---|---|
| Monopolizing the conversation | Invite others to share: "Let's hear if some other people have had a similar experience." |
| Argumentativeness | Reflect/validate the speaker's feelings; encourage him or her to use the group to get additional information or others' perspective on the issue. |
| Emotionality | Acknowledge their feelings; provide comfort (and tissues). Gently shift to another group member, but come back to "check in" with the emotional member when he or she has stopped crying. If the person is very upset, perhaps a facilitator could leave the group with him or her temporarily until he or she feels better. |
| Incorrect information | Don't directly challenge the information as false, but if there is no scientific evidence to support the information, say so. Invite the participant to discuss the issue with you later: "I have another explanation I'd like to share with you after group." |
| Lack of participation | Invite the member to share: "I notice you have been quiet through all of this; what are your feelings about (or your experience with) the issue?" |
| Rambling | Reflect that the speaker makes a number of good points; suggest the group focus on the most relevant point. |
| Interruption of the speaker with questions | If you have an invited speaker giving a lecture, point out that there is a lot of material to cover and suggest the group hold their questions until the end. |
Question and Answer Period
Even if you have decided to go with an educational or lecture-style format for your group, it is important to allow ample time for members to ask questions or share their comments on an issue. Some educational presentations are informal and allow for questions during the lecture, but often it's best to hold questions until after the speaker has presented all of his or her planned material.
The Social Aspect of Support Groups
Much of the strength of support groups is found in the patient-to-patient interactions that occur before, during, and after the official meeting. This is when veterans share information, compare notes, and even exchange phone numbers for informal contact outside of the group. While starting and ending groups on time is a good suggestion from a group management perspective, encouraging this peer-to-peer networking is important to promote patient self-help and to let the group thrive. Perhaps you can identify a safe, accessible place where patients can continue to talk even if your meeting room has to be locked up or released to the next scheduled user. If this is a possibility, announce to group members at the beginning of the meeting when the group officially ends and when and where informal discussions may continue.
Special Considerations for Hepatitis C and Liver-related Conditions Groups in Mixed Outpatient and Domiciliary Settings
- Confidentiality. Try to choose a space that allows for persons to enter unnoticed by the general population. Remember that hepatitis C is a disease that often carries a stigma. Domiciliary patients may choose not to attend rather than reveal their hepatitis C positive status.
- Frustration. Many veterans in a substance-use domiciliary will be frustrated if they are attempting to establish some sober time or to decrease their alcohol intake before starting treatment. Encourage veterans to use the time to prepare their bodies and minds for the treatment.
- Familiarity and Group Dynamics. Domiciliary patients often spend the majority of their time in each other's company. They may know each other well and have patterned ways of interacting throughout the many groups within the domiciliary program. This can affect the group dynamic in several ways you may not anticipate, especially if you are not domiciliary staff. You will need to establish the hepatitis C group as its own group, not just one of a number of domiciliary groups. Holding the group outside of the domiciliary (e.g., in an outpatient clinic) and including nondomiciliary patients can help establish this fact. Discourage participation of those who do not have hepatitis C by offering limited hepatitis C information in the other domiciliary health classes.
- Origin of Hepatitis C. Those who are newly diagnosed often question the origin of the virus or the source of their infection. Be cautious not to let this discussion get too far within the support group. It can lead to divisiveness within the group between those who obtained the virus from high-risk behaviors (e.g., IV drug use) and those who did not (e.g., a blood transfusion). Mixed populations are particularly susceptible to this dynamic as persons in the domiciliary often are early in recovery from drug or alcohol abuse and readily disclose high-risk behaviors.
7. Implement a Feedback Function
Debriefing Between Facilitators
Facilitators should meet immediately after the group, even if only for 10 minutes, to discuss what happened and develop plans for followup. Here are some topics you may want to cover during your debriefing:
- Clinical issues requiring followup (e.g., a participant discussed severe depression or suicidal ideation, seemed agitated, is likely to drop out prematurely)
- Process issues in the group (e.g., a participant who dominates the group or one who does not participate, scapegoating, deflection from emotional issues)
- Case formulations and intervention plans: developing therapeutic plans for individual participants and the group as a whole
- Follow up list of unanswered participant questions or requests for more information (e.g., referrals)
- Process issues between facilitators: mutual feedback, examining countertransference (i.e., personal reactions to group members), reaching agreements on practices, handling particular situations, responding to particular requests
Evaluating the Session
Feedback form
Using a standardized feedback form (see example in Appendix E) at the close of every group offers continuous feedback from participants to shape the group to their needs. Ideally, feedback should address four key aspects:
- Structure -- length, meeting times, formats
- Process -- facilitation style, issues between participants
- Content -- topics for guest speakers or focused discussions
- Expected outcomes -- how will group participants use the information
Data analysis
Once you solicit a group's feedback, it is extremely important to use that information. Let the group know at the outset that their feedback shapes the group, and then show them their feedback matters by altering the group accordingly.
Flexibility and Creativity
Groups are not set in stone and should change with the changing composition and needs of their members. Groups may change in purpose, focus, content, or structure. If one group seems to have outlived its usefulness, don't be afraid to end it and start a different type of group that might address patients' needs in a new way.
Reminder Calls and Letters
Reminders can work in a number of ways. One useful strategy is for facilitators to make the initial invitation to join the group face-to-face or by phone, then send members reminder letters before every group meeting. No-shows and drop-outs are common occurrences in groups, so facilitators should agree on a follow up plan for handling them. It is especially important to follow up with members who have expressed some important concerns or are having a particularly difficult time with their illness. If volunteer or peer facilitators are to contact members, the VA facilitator should ask members' permission first, guarantee their confidentiality, and clarify the limits on volunteers' access to the members' medical information.
Longstanding Groups
Just as your group may run its course and end naturally after fulfilling its usefulness, it may also become a mainstay of your health care facility. Don't be surprised if the group takes on a life of its own, with members developing their own rituals and traditions. Allow for the group to have alternative functions, such as holiday parties, participation in community events (e.g., local Liver Walks), or even reunions for very long-standing groups.
As one longtime support group member advises, stick with a generic name for the group. Your group may evolve over time and eventually look very different than it did when you held the first meeting.
Final Thoughts
Running groups can be extremely rewarding, as well as frustrating. Here are some parting tips on how to take care of yourself and avoid burnout:
- Network with other providers. Process and debrief challenges. Coordinate care with other providers and use a team approach. If some of your own issues emerge as a result of your helping others, seek counseling.
- Keep yourself abreast of new information by participating in ongoing education.
- Follow the advice that you teach to clients about physical, mental, emotional, social, and spiritual self-care. Self-care is the opposite of burnout.
- Recharge yourself! Pay attention to your personal time away from work and schedule activities that make you feel better. Set time aside for yourself. The more you enjoy your time away from work, the more you have to share at work.
- Recognize resentments against clients, colleagues, and work as signs that you are giving too much and not attending to your own needs.
- Set realistic goals for yourself at work. Keep reminding yourself, "It's not my job to save the world." Instead, focus on the smaller ways you can make it a better place today, if only for one person at a time.
- Know you are making a difference. Keep a file of all the thank you cards and commendations that remind you of the many people who appreciate what you do.
Appendixes
- Group Mission Statement (Sample)
- Support Group Meeting Planning Grid
- Group Participant Rights and Responsibilities
- Theories and Techniques for Support Group Facilitators
- Ongoing Support Group Evaluation Form
- Suggested Educational Topics
Appendix A
Group Mission Statement (Sample)
A support group serves to empower the patient through increased knowledge gained from speakers and other members as well as through the assurance that he/she is not going through his/her problem alone.
Appendix B
Support Group Meeting Planning Grid
| Program Title | |
|---|---|
| Meeting Date | |
| Location of Meeting | |
| Room Reserved | |
| Expected Attendance | |
| Speaker | |
| Facilitator(s) | |
| Program Title | |
| Agenda for Meeting | |
| Handouts | |
| Audiovisual Equipment | |
| Food/Refreshments | |
| Publicity/Plans | |
| Flyers/Newsletter | |
| Directions Posted | |
| Contact Person | |
| Program Organizer |
Appendix C
Group Participant Rights and Responsibilities
- We agree to participate in this program in a group setting with other patients and their families.
- We understand the need for complete confidentiality and trust within the group.
- We accept an individual's choice to actively participate or simply listen.
- We will begin and end meetings on time.
- We encourage "I" statements to keep discussions in the first person.
- We let one person speak at a time.
- We don't let one person monopolize the discussion.
- We recognize the importance of actively listening to the person who is speaking.
- We emphasize each individual's role in the group's success.
- We will not be judgmental toward other members; we are here to support, not criticize.
- We accept all feelings, whether they are positive or negative.
- We agree that each of us is responsible for our own comments and that we need to consider the group setting prior to disclosing personal information. We should keep in mind that some questions and comments may need to be presented in an individual session.
- We recognize and authorize that a participant's personal medical information may be disclosed in the group setting in order to respond appropriately to that participant's questions.
By my signature below, I show that I understand the purpose of this document.
Patient Signature
Facilitator Signature
Appendix D
Theories and Techniques for Support Group Facilitators
Stages of Group Development
Groups typically follow certain broad and overlapping stages of formation, growth, and decay (Corey Corey, 1997; Yalom, 1995):
- Beginning -- Trust is a central issue. Participants begin to learn what it means to be a member of the group, take tentative steps toward participating in the group, and observe and test others' reactions to them. The facilitator works to establish an emotionally supportive environment, fosters functional group norms, and validates feelings of fear, ambivalence, and alienation. Early facilitator interventions focus on acknowledging all participants' contributions and highlighting commonalities among participants.
- Transition -- Conflicts arise as participants see beyond their common goals to differences in styles of participating. Every group has conflict, but a group becomes therapeutic by bringing this conflict to the surface and resolving it directly and constructively. Conflict is a natural pathway of development and is necessary for the group to progress to cohesion. Participants become aware that to make progress in the group, they'll need to risk becoming vulnerable and to attempt new behaviors. Participants find their respective roles and places in the group. Facilitators' authority is often challenged. Facilitators must be keenly attuned to transference and countertransference and respond with process more than content in mind.
- Working -- By working through the conflicts of the transition stage, the group reaches a functional cohesiveness and trust through which it achieves its central goal. Participants feel a common bond, disclose more, participate more, mutually support each other, and actively facilitate the group's process. This stage is devoted to process, so educational/informational, open-enrollment, and nonprocess-focused groups may never reach this stage, and may not need to, in achieving their aims.
- Ending -- Participants acknowledge that the group will end and struggle with finding meaning and value in having participated even though it is ending. Participants identify and consolidate gains, as well as plan how to generalize their new behaviors in group to the rest of their lives. Participants may feel both happy about "graduating" and unhappy about losing the group. This is a time when old dysfunctional behaviors may reemerge. Participants may deny or minimize feelings of loss by saying they will keep in touch with other group members, but facilitators must help participants discuss the loss honestly.
Facilitation Techniques
Certain basic techniques are easily learned and quite useful in facilitating groups:
- 3 Rs of Listening -- Focusing on listening rather than preparing to respond to what is being said: preparing to listen (Readying), encouraging the speaker to say more (Reaching), and paraphrasing what the speaker has said (Reflecting).
- Immediacy -- Showing you're interested by making eye contact; nodding; reacting with other appropriate face, body, and vocal expressions; gesturing; and maintaining an appropriately close distance from the other person.
- Addressing by Name -- Calling people by their names establishes a personal connection and can help calm an agitated participant or focus one who is moving off task.
- "I" Statement -- A communication format focusing on the speaker's experience of the person being addressed: "I feel [emotion] when you [behavior]; I would prefer [alternate behavior] and/or [positive/negative consequences]."
- Giving Feedback -- Sharing how a participant's behavior personally affects you. The speaker should focus only on his or her personal reaction, focus on behavior over character or some attribute that is more difficult to change, be very specific by giving a concrete example, and use very recent examples.
- Confrontation -- Pointing out how a participant's behavior affects you (or others in group) and highlighting the possible consequences.
- Soliciting Feedback -- Asking others for their reaction to your behavior or that of a group participant.
- Paraphrasing (Reflecting) -- Restating a participant's words in a concise way. This shows people that you are listening and often helps them observe their own experience.
- Supporting -- Acknowledging people's experience and their right to feel however they do. This helps calm or soothe negative feelings.
- Labeling -- Helping a participant name a feeling he or she is experiencing.
- Perception Checking -- A three-part method for verifying the accuracy of interpretations, including a description of the observed behavior, at least one possible interpretation, and a request for confirmation of the interpretation. "I notice that you [sensory data/behavior]; to me that means [interpretation]; is that right (request for clarification)?"
- Self-Disclosure -- Revealing personal information about yourself to the participants. When a facilitator self-discloses, he or she should consider the goal in disclosing and plan on how much to disclose. Self-disclosure is a powerful tool in the early stages of group to help model such behavior and establish a group norm; however, the facilitator should be careful of disclosing too much, monopolizing the group, or using the group for personal reasons.
- Praising (Stroking) -- Calling attention to a specific positive behavior of a participant and how it affects others.
- Deflecting -- Rather than responding to a communication made directly to you (the facilitator), you open the discussion up to the group as a whole or to another specific participant. This is a way of encouraging cross-talk between participants rather than having each one interacting only with the facilitator. It is also a useful way of ending one participant's monopoly of group time and inviting others into the conversation. For example, "Has anyone else had a similar experience?"
- Punctuating -- Summarizing or making an observation as a way of stressing the importance of what has just happened or as a means of ending one train of discussion or speaker's time and starting a new one.
- Broken Record -- Repeating your statement calmly to get your point across.
- Using Silence -- Tolerating or fostering awkward pauses and silences in the group. This is one of the most useful group process techniques and one of the easiest ones to overlook for beginning facilitators. People naturally tend to be uncomfortable with silences and try to rush to fill the void with a new topic; however, the silences are often times when people are becoming aware of strong or anxiety-evoking feelings or are provoked into deep thought. Allowing a prolonged silence may deepen participants' experience of their feelings. By not "rescuing" the group from this discomfort, the facilitator may allow another participant to come forward and deepen or add to the conversation. If no participant comes forward after a long enough pause or if one attempts to move off the topic entirely, the facilitator can deepen the conversation by saying something like, "Although nobody spoke in the past few minutes, I know that everybody was thinking or feeling something that they didn't say. Would you please share what you were just feeling or thinking about?" You can build your tolerance for such silences by sitting with a group of friends or coworkers and agreeing to be silent for the next 1, then 2, then 3 minutes. You will observe a natural tendency to end the awkward silence by talking or laughing.
Motivational Interviewing
Miller and Rollnick (1991) articulated a nonconfrontational therapeutic approach to foster behavior change. Many have applied their approach to work with substance use disorders, but motivational interviewing is now proving effective with other health behavior change as well. They recommended five therapeutic principles or activities for assisting people to move toward behavioral change. These principles can be used in groups as well as individually.
- Express Empathy
- Listen to understand.
- Accept participants as they are.
- Ambivalence is a normal human experience.
- Reluctance to give up something that causes problems is normal.
- Joining (empathically siding) with the participant can foster change.
- Develop Discrepancy
- Becoming aware of a behavior's consequence is an important step toward changing it.
- Everything has good and bad consequences.
- Look for consequences in participants' adaptive coping, legal, health, work, and social contexts.
- Discrepancy between a behavior and important personal goals can foster change.
- Explore participants' personal goals.
- Participants develop the reasons for change themselves, rather than being told by the facilitator.
- Avoid Argumentation
- Arguments are counterproductive.
- Direct argumentation calls for a reaction from the participant.
- Saying "You can't" makes people want to assert their freedom by proving they can.
- Resistance signals a need to change your (the therapist's) strategy.
- Roll With Resistance
- "Psychological judo" -- Use the participant's inertia; sidestep an issue the participant is "dug in" on rather than butting heads with him or her.
- Perspectives can be shifted.
- The participant is an ally in solving the problem.
- Invite participants to try other perspectives, but don't impose them.
- The participant generates solutions: Ask, "What would you like to do about this?"
- Support Self-Efficacy
- Believing that someone can change motivates him or her (hope).
- Participants are actively making decisions about their lives (even when they decide not to change things).
- Participants (not the therapist) are responsible for choosing and making changes.
References
Corey, M.S., and G. Corey. Group Process and Practice. Pacific Grove, CA: Brooks/Cole, 1997.
Miller, W.R., and S. Rollnick. Motivational Interviewing: Preparing People for Change. New York: Pacific Press, 1991.
Rollnick, S., P. Mason, and C. Butler. Health Behavior Change: A Guide for Practitioners 11th Ed. Edinburgh: Churchill Livingstone, 1999.
Yalom, I. The Theory and Practice of Group Psychotherapy, 4th Ed. New York: Basic Books, 1995.
Appendix E
Ongoing Support Group Evaluation Form
| Today's date: | |||
| I am... | a veteran | a significant other | |
| For significant others: | |||
| I am... | HCV+ | HCV- | don't know |
| What information provided in this group was most helpful to you in understanding hepatitis C? | |||
| What was least helpful? | |||
| What topics would you like to see covered more or less extensively | |||
| What topics would you like to be added to the program? | |||
| How did these group sessions help you in understanding and coping with a diagnosis of hepatitis C? | |||
| What other changes, comments, or suggestions do you recommend? | |||
Thank you for your participation. Your answers will be used in further developing the group program.
Appendix F
Suggested Educational Topics
Many patients have indicated the following topics as being of particular interest to them. Support group planners may seek out guest speakers with specialized knowledge or expertise in these areas.
- Your Liver & Hepatitis C
- Understanding Lab & Biopsy Results
- Diet & Nutrition
- Managing Sleep, Fatigue, and Exercise
- Symptom & Side-effect Management
- Emotional Self-Care
- Anger Management
- Benefits & Service Connection
VA Hepatitis C Resource Centers published the first edition of this guide in October 2003.




















